Most people associate a tooth abscess with severe discomfort, swelling, or throbbing pain. While pain is a common symptom, it is not always present. In some situations, a tooth abscess or dental abscess can develop quietly, without obvious warning signs, until the infection becomes more advanced.
Understanding how an abscess can exist without noticeable pain, why this happens, and when to see your dentist can help protect your oral health and reduce the risk of complications.
What Is a Tooth Abscess?
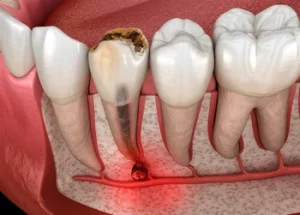 A tooth abscess is a pocket of infection caused by a bacterial infection. It develops when bacteria enter the tooth or surrounding gum tissue and begin to multiply. Over time, the body responds by forming pus, which creates pressure inside the area.
A tooth abscess is a pocket of infection caused by a bacterial infection. It develops when bacteria enter the tooth or surrounding gum tissue and begin to multiply. Over time, the body responds by forming pus, which creates pressure inside the area.
There are several types of abscesses, including:
- Periapical abscess, which forms at the tip of the tooth’s root
- Periodontal abscess, which develops in the gum tissue near the tooth
- Gum abscess, which affects the soft tissues surrounding the teeth
Any of these can become an abscessed tooth if left untreated.
How Can a Tooth Abscess Have No Pain?
Pain occurs when an infection irritates nerves or builds pressure in confined spaces. In some situations, the nerve inside the tooth becomes damaged or dies before pain is felt. When this happens, the abscess may continue to grow silently.
An abscess may also occur without noticeable pain if:
- The infection drains slowly instead of building pressure.
- The infection is spreading gradually into the surrounding tissues.
This is why a tooth abscess without pain does not mean there is no problem.
Common Causes of a Tooth Abscess With No Pain
Several underlying factors can allow an abscess to develop without obvious pain.
Tooth Decay and Dental Disease
Tooth decay is one of the most common causes of abscess formation. When decay reaches the inner layers of the tooth, bacteria can infect the dental pulp, leading to infection.
Over time, decay can result in an infected tooth without immediate symptoms.
Gum Disease and Poor Oral Hygiene
Gum disease allows bacteria to travel beneath the gum line. In cases of poor oral hygiene, bacteria can accumulate around the teeth and gums, increasing the risk of a periodontal abscess.
Prior Dental Work
In some cases, prior dental work such as fillings or crowns may weaken the tooth structure, allowing bacteria to enter small cracks and cause infection later.
Dry Mouth
Reduced saliva flow can increase bacterial growth. Ongoing dry mouth limits saliva’s natural cleansing effect, which increases the risk of tooth decay and abscess development.
Why an Abscess With No Pain Is Still Dangerous
A tooth abscess without pain can be more dangerous because it is easier to ignore. Without treatment, the infection may worsen.
If left untreated, an abscess can:
- Spread into the surrounding tissues.
- Affect nearby blood vessels.
- Lead to serious complications.
- Damage the jawbone or neighbouring teeth.
- Result in tooth loss.
In rare cases, the infection can spread beyond the mouth, causing facial swelling or systemic illness.
Signs to Watch for When There Is No Pain
Even without pain, there are warning signs that should not be ignored:
- Facial swelling or mouth swelling

- A small pimple-like bump on the gums
- Tender lymph nodes or swollen lymph glands
- Bad taste or persistent bad breath
- Tooth sensitivity to pressure or temperature
- Changes in gum colour or texture
- General feeling of discomfort in the jaw or face
In more difficult situations, symptoms may include difficulty swallowing or difficulty breathing, which require urgent medical care.
Types of Tooth Abscess Explained
Abscesses vary based on where the infection begins and spreads.
Periapical Abscess
A periapical abscess forms when bacteria reach the pulp through decay or cracks. This type often starts inside the tooth and spreads to the root tip.
Periodontal Abscess
A periodontal abscess develops in the gums and is commonly linked to gum disease. It involves the tissues that support the tooth, rather than the tooth pulp itself.
Gum Abscess
A gum abscess forms in the soft gum tissue and may not involve the tooth pulp initially, making it easier to miss.
Tooth Abscess Treatment Options
The goal of tooth abscess treatment is to remove the infection and prevent further damage.
Root Canal Treatment
Root canal treatment removes infected pulp from inside the tooth, cleans the canal, and seals it. This option may allow the natural tooth to be preserved.
Tooth Extraction
If the tooth is too damaged, removal may be required. This ensures the infection does not continue to spread.
Drainage of the Abscess
In certain situations, a dentist may release the built-up fluid to relieve pressure and clear infected material.
Once a tooth abscess is treated appropriately, healing can begin, and the risk of complications is reduced.
What Happens If an Abscess Is Ignored?
Ignoring an abscess that causes no pain allows the infection to continue progressing beneath the surface. While symptoms may remain mild at first, the underlying damage can increase over time.
As the infection advances, it may:
- Reduce the likelihood of saving the affected tooth
• Require more complex treatment than initially needed
• Increase healing time once treatment begins
• Lead to sudden flare-ups of pain or swelling
• Disrupt daily activities such as eating or sleeping
Delaying care can also limit treatment options, meaning more invasive procedures may be required later.
Early dental care helps control infection sooner, preserve more natural tooth structure, and reduce the risk of sudden complications.
When to See a Dentist
You should see a dentist if you notice any signs of infection, even without pain. Seek help as soon as possible if symptoms worsen.
Contact your dentist as soon as you notice:
- Swelling
- Changes in gum tissue
- Persistent bad taste
- Signs of infection
In emergencies involving breathing or swallowing difficulties, urgent care should not be delayed.
Preventing Tooth Abscesses
While not all abscesses can be prevented, good habits reduce risk.
Maintain Good Oral Hygiene
- Brush with a soft toothbrush.
- Clean carefully along the gum line.
- Use fluoride toothpaste.
- Rinse with a fluoride mouth rinse or fluoride mouth product if recommended.
Support Dental Health
- Attend regular dental check-ups.
- Address decay early.
- Treat gum disease promptly.
- Maintain overall dental health.
Reduce Risk Factors
- Manage poor dental hygiene.
- Address dry mouth symptoms.
- Monitor areas with prior dental work.
These steps help protect oral health and reduce the chance of abscess formation.
Tooth Abscess With No Pain Does Not Mean No Risk
A tooth abscess without pain can still cause significant harm. The absence of pain does not mean the infection is harmless or resolving on its own.
Because an abscess can affect surrounding structures, early detection and professional treatment are essential.
Final Thoughts
 Many factors, such as tooth decay, gum disease, and untreated dental infections, can lead to a tooth abscess. No pain may be present in the early stages, even though infection is developing.
Many factors, such as tooth decay, gum disease, and untreated dental infections, can lead to a tooth abscess. No pain may be present in the early stages, even though infection is developing.
If you notice swelling, changes in the gums, or other warning signs, seeking dental care promptly helps reduce the risk of complications. Early care protects your teeth, gums, and overall health, and helps prevent serious complications from developing.
If you’re concerned about signs of a tooth abscess without pain or want clarity on changes you’ve noticed in your mouth, you can book a consultation with us at Sure Smile Dental or call (07) 3185 2387 to discuss your oral health and receive personalised guidance.
Note: Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
Resources
Pietrangelo, A. (2024). ‘Why Do I Have a Bad Taste in My Mouth?’. Healthline, 17 January. San Francisco, CA: Healthline Media. https://www.healthline.com/health/bad-taste-in-mouth
Mayo Clinic Staff (2025). ‘Root canal treatment’. Mayo Clinic, 5 September. Rochester, MN: Mayo Foundation for Medical Education and Research. https://www.mayoclinic.org/diseases-conditions/tooth-abscess/in-depth/root-canal/art-20585454
Cleveland Clinic (2023). ‘Dry Mouth (Xerostomia)’. Cleveland Clinic, last reviewed 15 September. Cleveland, OH: Cleveland Clinic Foundation. https://my.clevelandclinic.org/health/diseases/10902-dry-mouth-xerostomia






Recent Comments